Psychodermatology: A Review
Psychodermatology has a prominent presence within the field of dermatology. In a typical dermatology practice, 30 to 40 percent of patients experience psychological problems in relation to their dermatological symptoms.1 Although psychodermatological issues are commonly encountered in clinical practice, the lack of familiarity and comfort of dermatologists with regard to the diagnosis and management of patients’ psychological concerns has led to their frequent disregard in the field. Referrals to psychiatrists or other mental health professionals are often declined or taken offensively by patients.1 Thus, the dermatologist must often address the issue himself, lest it never be addressed. Because residents’ education rarely covers psychodermatology, dermatologists often find themselves unable to manage these patients with confidence. This review aims to provide a review and practical recommendations in the categorization and management of common psychodermatological problems.

Figure 1. Classification system of psychodermatology. Psychodermatology can be classified by the different categories of psychodermatological problems or by the nature of the underlying psychopathology.
Classification
Psychodermatology is a comprehensive field inclusive of multiple types of disorders. A systematic classification system has been developed to understand the field in its entirety.1,2 This is unique to psychodermatology, as this classification system is not entirely represented in the DSM V. For example, DSM V does not include diagnostic codes for the exacerbation of skin diseases with emotional stress.
There are two major ways to classify psychodermatology: 1.) by different categories of psychodermatological problems and 2.) by the nature of the underlying psychopathology (Figure 1).2
Classification by psychodermatological categories. With regard to classification by different categories of psychodermatological disorders, there are four main categories: psychophysiological disorders, primary psychiatric disorders, secondary psychiatric disorders, and cutaneous sensory disorders.3 Although these are four separate categories, they are not mutually exclusive, as a single case may qualify for multiple categories.
Psyschophysiological disorders. Psychophysiological disorders consist of bona fide organic dermatological conditions that are frequently exacerbated by emotional stress.3 Though stress is purely psychological, it can cause patients to experience an increase in the frequency and intensity of skin symptoms. This is the dermatological equivalent of conditions such as peptic ulcer disease and migraines, in which the onset and natural course can be changed based on the emotional state of the patient. Examples of skin conditions that are frequently affected by stress include atopic dermatitis, psoriasis, acne vulgaris, lichen simplex chronicus, rosacea, and seborrheic dermatitis. There are also common conditions where inflammation is not obviously visible but may still be worsened by stress, such as alopecia areata and hyperhidrosis. Patients with these conditions can be separated into two subgroups, referred to as “stress responders” and “non-stress responders.”4 The proportion of stress responders versus non-stress responders varies by condition, ranging from 100 percent stress responders in hyperhidrosis to zero percent stress responders in skin carcinomas.4 Furthermore, the time of onset of clinical symptoms from the initial stress trigger can range by disease from seconds to multiple days. For example, in atopic dermatitis, 70 percent of the patient population responds to an emotional trigger that almost immediately results in increased pruritis.4 Whereas 62 percent of psoriasis patients take a few days to respond to stress and show clinical change.4
Primary psychiatric disorders. Primary psychiatric disorders are diagnosed in patients who present with skin lesions that are self-induced in the absence of organic etiology.3 These patients have normal, non-diseased skin, hair, and nails. All skin lesions are self-inflicted even though the patients often are convinced that they have a real skin disorder. Although their symptoms are the manifestation of the patient’s underlying psychiatric condition, patients are less likely to accept referral to a psychiatrist or to willfully take psychiatric medications. Primary psychiatric disorders include neurotic excoriations, factitial dermatitis, trichotillomania, onychotillomnia, and delusions of parasitosis.
Secondary psychiatric disorders. Secondary psychiatric disorders are psychological problems that develop secondary to the negative impact of skin disease on the patient’s psyche.3 Nearly always, the disfigurement caused by skin disease has a profound impact on a patient’s psychological welfare. In conditions such as vitiligo or alopecia areata, patients struggle with the psychosocial impact of the disease more than with the symptoms.
Cutaneous sensory disorders. Cutaneous sensory disorders are conditions in which the patient experiences various abnormal sensations on the skin.5 However, internal workup is negative and the patient lacks a diagnosable primary skin disorder. The sensations experienced include, but are not limited to, itching, burning, stinging, biting, and crawling, and can be found in any anatomic locations.5 Terminology has been developed to identify the sensation in specific body parts; for example, glossodynia and vulvodynia refer to the cutaneous sensory disorder in the mouth and the vulva, respectively. A common scenario includes a male patient who experiences chafing or burning sensations in his groin for which no dermatologic or medical finding can be identified. This category can be seen as the skin equivalent of chronic pain syndrome. A psychiatric diagnosis may or may not exist for these patients. If one is present, it is often anxiety or depression.
Classification by psychopathology. With regard to the categorization of pyschodermatology by the underlying psychopathology, there are four psychiatric diagnoses that are most commonly encountered in dermatological practice: delusion, anxiety/stress, depression, and obsessive-compulsive disorder (OCD).3 These categories are not mutually exclusive, and many psychiatric conditions have been found to co-exist with one another. Diagnosis of these psychiatric conditions follows the DSM V guidelines, and can be managed with the appropriate psychopharmacology. Delusions are false ideas that patients accept as absolute truth, despite rational argument such as the presentation of opposing evidences. Anxiety and stress is characterized by subjective symptoms of tension, agitation, unease, and an inability to relax.6 Depression is diagnosed in patients who experience a depressed mood, crying spells, anhedonia, hopelessness, and a sense of worthlessness.6 Depression can also manifest as physical symptoms such as insomnia, hypersomnia, loss of appetitie, or hyperphagia. Lastly, OCD is seen in patients who suffer from intrusive obsessive thoughts with compulsive behaviors. OCD patients are different than delusional patients in that they are fully aware of their irrational behavior and often desire help. This is defined as “ego-dystonic.”6 This is in stark contrast to the “ego-syntonic” delusional patients who are unaware of the irrationality of their behavior and adamant their beliefs represent reality.
Commonly encountered psychodermatological disorders
Delusions of parasitosis. Delusions of parasitosis (DOP) is one of the most challenging psychodermatologic conditions for dermatologists, who often find it difficult to manage these patients. The condition has been referred to as acarophobia, Ekbom syndrome, parasitophobia, delusional infestation, and Morgellons syndrome.7
Definition. DOP is found in patients who have a fixed, false belief that they are infected with parasites or other living organisms.8 The classical form of DOP defines it as an “encapsulated” delusion, or the sole delusion that the patient experiences.9 With the exception of his DOP, the patient is relatively normal and does not have additional psychiatric findings. However, the diagnosis of DOP has also been given to patients with more global psychiatric disorders. Depending on the underlying global psychiatric disorder, such as organic brain syndrome or schizophrenia, these patients may exhibit additional psychiatric symptoms such as hallucinations, inappropriate affect, etc. We will be addressing DOP in its classical definition.
The primary symptom of DOP is formication, which is the term used to describe the sensation of bugs crawling on the skin.8 Because they maintain a fixed delusion that their condition is of dermatological etiology, these patients are reluctant to see a psychiatrist. The mere suggestion of a referral to a psychiatrist may create feelings of resentment and anger towards the dermatologist, often severing the patient-doctor relationship. These patients insist on being treated by a dermatologist.
Epidemiology. On average, a dermatologist will see two to three patients presenting with DOP every five years. The ratio of male-to-female patients with DOP is 1:1 in patients less than 50 years of age.10 However, in patients older than 50 years of age, which represent the majority of cases, DOP is found in females 2.5 times more frequently than in males. Similar to schizophrenia, age distribution is bimodal, with a peak prevalence in patients 20 to 30 years of age and in patients older than 50 years of age.10 Moreover, about five to 15 percent of patients with DOP will have a friend or relative with the same symptoms. This is known as folie a deux, which means “craziness for two.”10
Differential diagnoses. The initial step in the diagnosis of DOP is to differentiate it from primary psychosis secondary to schizophrenia. Unlike schizophrenics, patients with classic DOP do not experience multiple psychological impairment beyond their fixed delusion.11 If a patient presents with DOP, one should confirm that the delusion is encapsulated. As stated earlier, patients that experience other psychological symptoms may instead have a more global psychiatric derangement.
Substance abuse may cause similar psychosis. In addition to narcotics and amphetamines, cocaine is well known to cause a prominent crawling sensation underneath the skin, or “cocaine bugs”. Depression with psychosic (psychotic depression) may cause patients to feel “contaminated” with lice or mites. However, unlike patients with DOP, these patients express additional symptoms of depressed mood, ahedonia, and difficulty sleeping.
Underlying medical conditions may cause similar sensations. Vitamin B12 deficiency results in paresthesia that may be mistaken for DOP. Dorsalis tables secondary to tertiary syphilis can also cause paresthesia in addition to a lack of vibration or position sense. Advanced diabetes can cause sensorycutaneous disorders similar to formication.
Pharmacotherapy. Although the first line of treatment for DOP is antipsychotics, it is important to establish good therapeutic rapport before approaching this medication use. Once this has been established, there are both typical and atypical antipsychotics that can be prescribed for DOP. Pimozide (Orap®) is a typical antipsychotic that has been considered the gold standard for treatment of DOP historically.13 Pimozide is approved by the FDA for Tourette syndrome, which is a neurological disorder, and lacks an official indication for any psychiatric disorder. Because DOP patients are reluctant to agree that they have a psychiatric disorder, the lack of an official psychiatric indication will make the medication more acceptable to these patients. A possible side effect of pimozide and other typical antipsychotics to consider are extrapyramidal side effects (EPS).
Atypical antipsychotics block both the serotonin and dopamine receptors. Risperidone (Risperdal®) is the second most studied atypical antipsychotic for DOP and has shown excellent efficacy for treating DOP. Both aripiprazole (Abilify®) and quetiapine (Seroquel®) have also shown efficacy in treating DOP and are recommended based on their mild safety profile.12
Neurotic excoriations
Although “neurotic” is part of the diagnostic label, neurotic excoriations do not necessarily represent neurosis in a patient. The patient may suffer from a variety of underlying psychiatric illnesses, including depression, anxiety, and OCD. Due to the various possible etiologies, “neurotic” excoriations has also been referred to as psychogenic exocriations.5
Definition. Neurotic excoriations are found in patients without primary skin disorder and present with self-inflicted excoriations, most commonly caused by an underlying psychiatric disorder including anxiety, OCD, or depression.14 The anatomical distribution of the excoriations is often indicative of the disease, as they are found in areas that are easily accessible. As a result, the bilateral upper, lateral back areas are commonly spared, a pattern referred to as the “butterfly sign (Figure 2).”15,16 In addition, patients tend to have a more prominent involvement of the lateral arm as compared to the medial arm, as well as the anterior thigh as opposed to the posterior thigh (Figure 3).15,16 The lesions may be excoriations or erosions, and are often found to be scabbing and crusting. There may be surrounding hyperpigmented or hypopigmented scars from previous self-inflicted wounds.
Patients often have an impaired impulse control and are unable to prevent themselves from inflicting the excoriations on their body.14 They may or may not acknowledge the self-inflicted nature of the lesions, especially on the first visit. Once rapport is established, they are more likely to admit to self-inducing them.
Epidemiology. Approximately 2 percent of dermatologic clinic patients suffer from neurotic excoriations, with females affected more often than males. The female-to-male ratio is controversial and has been reported to be anywhere between 1:1 to 8:1. The mean age of onset is from 30 to 45 years.14
Differential diagnoses. In approaching the differential diagnosis for neurotic excoriations, one must consider both medical and psychiatric etiologies. First, it must be confirmed that there is no primary skin disease. The management relies on the underlying psychiatric diagnosis. Thus, except in delusional cases, it is important to ask the patient for current symptoms of psychiatric disorders.
Depression is a possible underlying cause of neurotic excoriations. Following the DSM-V definition for diagnosis of a major depressive episode, patients may present with anhedonia, crying episodes, a depressive mood, loss of appetite, or loss of sleep.6 Obsessive-compulsive disorders are egodystonic, and the patient is often aware of their inability to resist the impulsive behavior.6 These patients often actively seek help. Patients with anxiety often appear stressed, apprehensive and irritable. These feelings are often manifested as physical symptoms such as tachycardia and repetitive fidgeting movements, including the picking of the skin characteristic of neurotic excoriations.

Figure 2. Characteristic distribution of neurotic excoriations. Neurotic excoriations commonly spare the bilateral upper and lateral back areas due to difficult access, a pattern known as the “butterfly sign.”
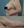
Figure 3. Characteristic distribution of neurotic excoriations on the arms. The excoriations are found more prominently on the lateral arm (A). However, the medial arm is often spared due to positioning difficulties (B).
Pharmacology. Once the psychological etiology for the disease is diagnosed, the appropriate pharmacology can be prescribed. If the patient experiences anxiety, benzodiazepines may be used. SSRIs are the first line treatment for depression and obsessive-compulsive disorder. In a rare delusional case, antipsychotics are recommended.
Despite the psychiatric etiology of neurotic excoriations and lack of a primary skin disorder, patients may bitterly complain of pruritis. Topical anti-pruritic, agents such as Sarna lotion or doxepin 5% cream (Zonalon®) may proivde symptomatic relief. Oral antihistamines such as hydroxyzine (Atarax®) or diphenhydramine (Benadryl®) may also be used for pruritus. In addition, doxepin can be taken orally as an antidepressant with the additional benefit of strong antipruritic, and antianxiety effects. Due to the ulceration of the epithelial barrier, the lesions must be assessed for possible infection. Topical antibiotics such as mupirocin 2% ointment (Bactroban®) or oral antibiotics such as cephalexin will help prevent and treat infections. Dressings that promote wound healing, such as DuoDERM®, may also be applied to the excoriated sites for faster healing.
Trichotillomania
Trichotillomania is a common primary psychiatric disorder that has been recognized in the DSM-V as a type of obsessive-compulsive spectrum disorder.6
Definition. Trichotillomania is characterized by the repetitive act of hair pulling which results in significant hair loss. As defined by the DSM-V, patients with trichotillomania must experience tension and discomfort when attempting to resist the act, which is resolved with the additional feeling of pleasure and relief after the act is completed.6 Alternatively, dermatologists do not use the above strict requirements as specified in the DSM V. Any patient may be diagnosed with trichotillomania simply for pulling out his or her hair. Moreover, association with OCD is not required, as patients may have an underlying diagnosis of anxiety, depression, or, rarely, delusion known as “trichophobia.”17 They may also be only partially aware of their behavior, and may be unwilling or ashamed to verbally acknowledge the self-induced nature of the condition.
The most commonly involved body parts are the scalp, eyelashes, eyebrows, and pubic hair. Patients may experience hair loss in more than one area. The area of hair loss commonly presents without scarring and instead with a patch of short, sparse hair distinct from the rest of the scalp. Histopathology can be confirmatory. Findings that may be helpful in making the diagnosis include an increased number of catagen hairs, melanin pigment casts, and traumatized hair bulbs without significant perifollicular inflammation (trichomalacia).17
Epidemiology. It has been reported that approximately three to eight million individuals in the US are affected by trichotillomania.5 The disorder is much more prevalent in females than males, and has an average initial onset age of 10 to 13 years.17 Hair pulling behavior, which may or may not meet the DSM V criteria for trichotillomania but is still diagnosed as “trichotillomania” by dermatologists, is present in the female to male population at approximately a 9:4 ratio.5,17
Differential Diagnosis. Trichotillomania must be differentiated from OCD. According to the DSM V, patients with OCD do not gain pleasure from their act, and instead find it unpleasant but irresistible.6 However, trichotillomania patients find the act of hair pulling gratifying and as a way to relieve feelings of anxiety or tension.
Pharmacotherapy. Trichotillomania is treated with SSRIs, which are also used to treat OCD. Paroxetine (Paxil®), sertraline (Zoloft®), fluoxetine (Prozac®), citalopram (Celexa®), and escitalopram (Lexapro®) can be prescribed as monotherapy for trichotillomania. The tricyclic antidepressant (TCA) clomiprmaine (Anafranil®) has also shown efficacy in treating trichotillomania.18
Atypical antipsychotics such as aripiprazole and risperidone have been used in combination with SSRIs or as monotherapy for refractory trichotillomania.18 Antiepileptics such as carbamazepine (Tegretol®) and oxcarbazepine (Trileptal®) has been recently reviewed for use in impulsive-control disorders. However, their use for trichotillomania remains controversial.19
Secondary psychiatric disorders
Secondary psychiatric disorders are problems resulting from the disfigurement of a primary skin disorder.5 Patients with skin disorders such as vitiligo and atopic dermatitis often suffer from a significant negative psychological impact, though usually not severe enough to qualify as a mental illness. Dermatologists are often challenged to justify the significance of their intervention. As a response, it has been documented that the physical deformities from skin disease cause a decline in patients’ quality of life, and can lead to severe depression, anxiety, and social phobia.2 Because of society’s focus on outward appearance, “cosmetic” defects can even carry a much larger psychological impact than that of an internal but life-threatening diseases such as diabetes or hypertension, which are not readily visible.22
Social stigma also plays a role in exacerbating the psychosocial impact of skin disorders.22 The inability of the general public to distinguish between contagious diseases and a non-contagious skin disorder can lead to the social isolation of patients, negatively impacting their self-esteem. It is the dermatologists’ role to consider both the physical and emotional stress that skin disease places on a patient, and to take a comprehensive approach to the disease. Although a patient may present with mild disease, one may consider placing the patient on more aggressive therapy than the usual standard if he or she displays severe emotional distress from the disease. Similarly, a patient with severe disease but minimal emotional impact can find a less aggressive treatment option to be sufficient. Overall, the physical characteristics of a patient’s skin disorder alone should not dictate the type of treatment that should be provided due to consideration of the psychological aspect of the disorder.
Psychopharmacology
As psychopharmacology is a comprehensive field, a discussion of the topic as a whole is beyond this short review. This review will address the first line choice of therapy for various psychodermatological conditions and briefly cover their risks and benefits (Table 1).
In determining the first line therapy for pyschodermatological conditions, one must first consider the nature of the underlying psychopathology.5 Whenever possible, it is encouraged to consider both psychopharmacology and nonpharmacologic approaches such as psychotherapy, behavioral therapy, cognitive therapy, and group therapy.5 However, in the reality of dermatology practice, a multidisciplinary approach is usually not realistic. This is due to both the unwillingness of the patient to attend psychotherapy and the unfamiliarity of dermatologists with nonpharmacologic treatments. Because many of these patients refuse to be seen by any mental health professional, psychopharmacotherapy provided by a dermatologist as a single modality of treatment is likely to still be superior to the lack of any treatment.
Antipsychotics. Antipsychotics can be used to treat patients with DOP and those with underlying psychosis causing their symptoms. Both typical and atypical antipsychotics can be used. Typical antipsychotics have a higher affinity for dopamine receptors than the atypical class.23 Thus, they have been shown to have greater efficacy in treating DOP. Pimozide is a typical antipsychotic that is historically the first line therapy for DOP.13 However, atypical antipsychotics have a lower risk of EPS.23 Risperidone is an atypical antipsychotic that is commonly prescribed, and favored due to its milder side effect profile. Other atypical antipyschotics include aripiprazole, quetiapine, and olanzapine (Zyprexa®).
Antidepressants. There are a variety of available antidepressants extending beyond the breadth of knowledge expected of a dermatologist. Thus, it is recommended that dermatologists focus on increasing their comfort level with a few select agents. Paroxetine is an SSRI which has fewer side effects than TCAs.24 The strength of paroxetine lies in its ability to treat multiple psychiatric disorders beyond depression, including anxiety and OCD. However, once a patient is started on paroxetine, it is imperative that he or she do not abruptly discontinue it and instead taper the drug to avoid SSRI withdrawal symptoms and possible increased risk of suicide.

Antianxiolytics. Paroxetine is also recommended at lower doses as an antianxiolytics due to its lack of addictive properties. Buspirone (Buspar®) maintains a high safety profile when taken on a regular basis, but does not take effect until at least one month after the initial dosage. It must be taken on a regular dosing schedule, and is not effective if taken on an as needed basis. Alprazolam (Xanax®) is recommended for short term use due to its potentially addictive properties. It is advantageous due to its quick acting nature and relatively short half-life, preventing its accumulation in the body.25 Because alprazolam has a short half-life, it is important to avoid abruptly discontinuing the medication and to instead taper the medicine off gradually.
Anti-Obsessive compulsive disorder medications. For OCD, paroxetine is one useful option.24 A higher dosage is needed, and the patient must be warned of its slow onset of action which may take a month or longer. Thus, the dermatologist and patient must not become discouraged if the patient does not show improvement on a low dose; the dose may merely need to be titrated upwards.
Conclusion
Psychodermatological issues are commonly encountered in ordinary dermatological practices. Many psychodermatological patients refuse to be seen by a mental health professional and approach the dermatologist with hopes of receiving help. For these patients, especially those with a severely disabling condition like DOP, it is important for dermatologists to address their concerns, as the patient may not receive help otherwise. This review covers basic knowledge on psychodermatology, and hopes to assist dermatologists to provide empathetic and more effective care to these patients. With an increased awareness and comfort level amongst dermatologists with commonly encountered psychodermatological conditions, it is our hope that patients will no longer feel neglected and will instead foster a strong bond of trust with their dermatologist. n
No funding was received for this article. The authors have no conflict of interest to declare.
Catherine Nguyen is a medical student at University of California, Irvine School of Medicine who is currently a clinical research fellow at the UCSF Psoriasis, Phototherapy & Skin Treatment Clinic under Dr. John Koo, who is double-boarded in both dermatology and psychiatry.
Melissa Danesh, BS, University of California, San Francisco School of Medicine.
Kourosh Beroukhim, BS, David Geffen School of Medicine at UCLA.
Eric Sorenson, BS, USC Keck School of Medicine
Argentina Leon, MD, University of California, San Francisco Psoriasis Center.
John Koo, MD, University of California, San Francisco School of Medicine.
1. Jafferany M, Vander Stoep A, Dumitrescu A, et al: The knowledge, awareness, and practice patterns of dermatologists toward psychocutaneous disorders: results of a survey study. Int J Dermatol 2010; 49:784-789.
2. Koo JYM, Lee CS: Psychocutaneous Medicine. Basic and Clinical Dermatology. New York, Marcel Dekker, 2003; 1-12.
3. Koo JYM, Lee CS: General approach to evaluating psychodermatological disorders. In: Koo JYM, Lee CS: Psychocutaneous Medicine. Basic and Clinical Dermatology. New York, Marcel Dekker, 2003; 1-12.
4. Gupta MA, Gupta AK, Ellis LN, et al: Some psychosomatic aspects of psoriasis. Adv Dermatol. 1990; 5:21-30.
5. Koo JYM: Psychodermatology: A Practical Manual for Clinicians. Current Problems in Dermatology. Missouri, Mosby, 1995; 7:199-234.
6. Diagnostic and Statistical Manual of Mental Disorders, 5th ed. Text Revision. Washington, DC, American Psychiatric Association, 2013.
7. Bewley AP, LEpping P, Freudenmann RW, et al: Delusional parasitosis: time to call it delusional infestation. Br J Dermatol 2010; 163:1-2.
8. Freudenmann RW, Lepping P: Delusional infestation. Clin Microbiol Rev 2009; 22:690-732.
9. Freudenmann RW, Lepping P: Second-generation antipsychotics in primary and secondary delusional parasitosis: outcome and efficacy. J Clin Psychopharmacol 2008; 28:500-508.
10. Wykoff RE: Delusions of parisitosis: a review. Rev Infect Dis 1987; 9:433-437.
Koo JYM, Lee CS: Delusions of parasitosis. A dermatologists’ guide to diagnosis and treatment. Am J Clin Dermatol 2001; 2:285-290.
11. Lepping P, Russell I, Freudenmann RW: Antipsychotic treatment of primary delusional parasitosis: systematic review. Br J Psychiatry 2007; 191:198-205.
12. Riding BE, Munro A: Letter: Pimozide in monosymptomatic psychosis. Lancet 1975; 1:400-401.
13. Arnold LM, Auchenbach MB, McElroy SL: Psychogenic excoriation. Clinical features, proposed diagnostic criteria, epidemiology and approaches to treatment. CNS Drugs 2001; 15:351-359.
14. Brodin MB: Neurotic excoriations. J Am Acad Dermatol 2010; 63:341-342.
15. Cyr PR, Dreher GK: Neurotic excoriations. Am Fam Physician 2001; 64:1981-1984.
16. Duke DC, Keelye ML, Gefflen GR, et al: Trichotillomania: A current review. Clin PSychol Rev 2010; 30:181-193.
17. Epperson CN, Fasula D, Wasylink S, et al: Risperidone addition in serotonin reuptake inhibitor-resistant trichotillomania: three cases. J Child Adolesc Psychopharmacol 1999; 9:43-49.
18. Huband N, Ferriter M, Nathan R, et al: Antiepileptics for aggression and associated impulsivity. Cochrane Databse Syst Rev 2010; 17:CD003499.
19. Lai CS, Lee SS, Yeh YC, et al: Body dysmorphic disorder in patients with cosmetic surgery. Kaohsiung J Med Sci 2010; 26:478-482.
20. Phillips KA, Dufrescne RG: Body dysmorphic disorder. A guide for dermatologists and cosmetic surgeons. Am J clin Dermatol 2000; 1:235-243.
21. Koo JYM, Smith LL: Psychological asepcts of acne. Pediatric Dermatol 1991; 8:185-188.
22. Buchanan RW, Kreyenbuhl J, Kelly DL, et al: The 2009 schizophrenia PORT psychopharmacological treatment recommendations and summary statements. Schizophr Bull 2009; 36:71-93.
23. Gupta MA, Gupta AK: The use of antidepressant drugs in dermatology. J Eur Acad Dermatol venereal 2001; 15:512-518.
24. Lee CS, Accordino R, Howard J, Koo JYM: Psychopharmacology in dermatology. Dermatol Ther 2008; 21:69-82.
Ready to Claim Your Credits?
You have attempts to pass this post-test. Take your time and review carefully before submitting.
Good luck!





