PracticalDermatology

Herbals in the Holistic Treatment of Psoriasis
As patients’ interest in the option to incorporate alternative medicine (AM) into standard medical practice has grown, the medical community has responded in several ways: by beginning to teach related curriculum in medical schools and producing and distributing patient-directed interactive media. A survey of 130 US Medical schools found that around half offered at least one complementary and alternative medicine course or clerkship.1 As evidence of the worth of these efforts, a recent systematic review of the use of complementary and alternative medicine in the general population found that between 34 and 42 percent of Americans have used at least one AM product over a 12 month period.2 These numbers are consistent with what Eisenberg et al. found almost two decades ago, proving that the public’s pursuit of alternative therapies for medical conditions remains strong.3 Results from the most recent National Health Interview Survey, released in 2012, estimated out-of-pocket expenditures for AM in the year 2007 at $33.9 billion.4 Comparatively, $286.1 billion were projected as out-of-pocket expenses for physician services accrued during the same year.5 Reasons stated by patients for using AM include “willingness to do anything, dissatisfaction with ‘standard therapies’ and failure of conventional therapies.”6
It is estimated that only approximately 40 percent of the patients who practice AM (herbals) report this to their physicians,7 often not disclosing information regarding the use of alternative therapies because they do not consider herbals to be pharmacologic (e.g.: a drug with exerts a desired effect on an end organ). Contrary to this, not only are herbals pharmacologic, but they have the potential to significantly interact with prescribed conventional medications.
Psoriasis affects approximately 3.2 percent of the population in the United States (a number estimated as 7.4 million in 2013).8 As an indicator of the importance of alternative therapies in the lives of patients living with psoriasis (e.g.: herbal treatments, dietary manipulation, vitamin treatments), recent surveys indicated the prevalence of AM use in these patients between 42 and 69 percent.9 Patients may combine herbal therapies with standard medical therapies for psoriasis, at times employing alternative or herbal modalities without discussing or disclosing their use to their health care provider.
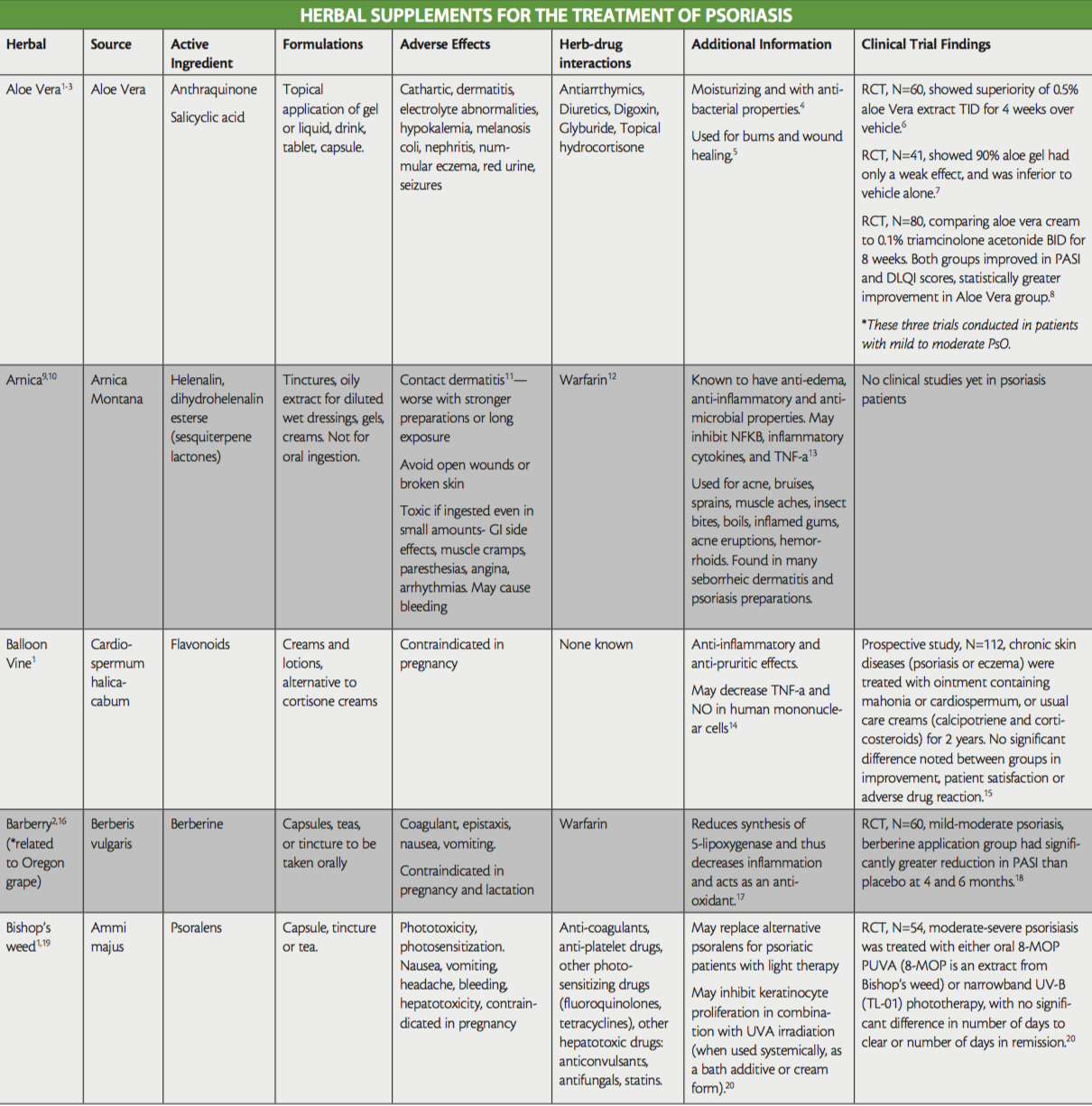
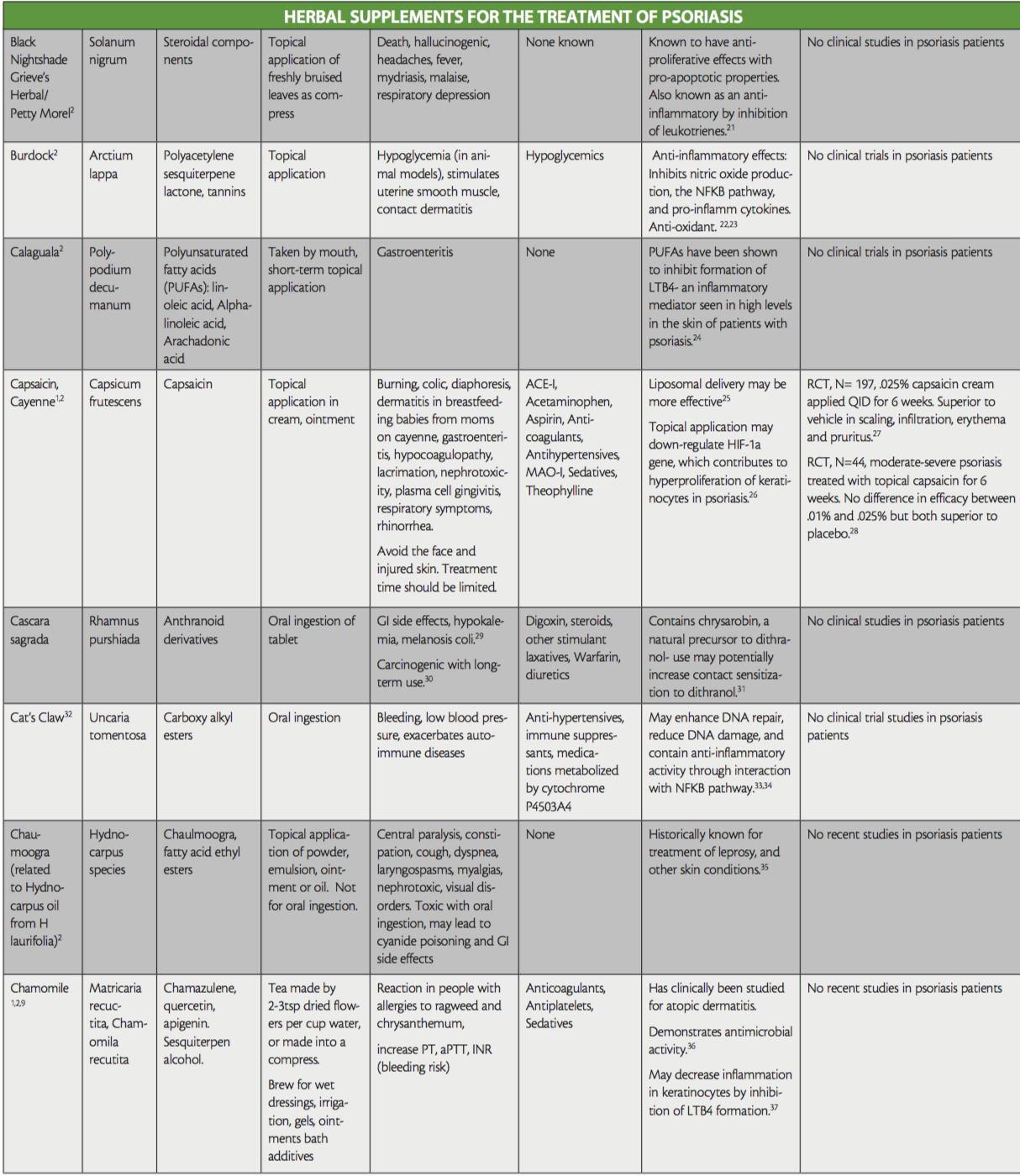
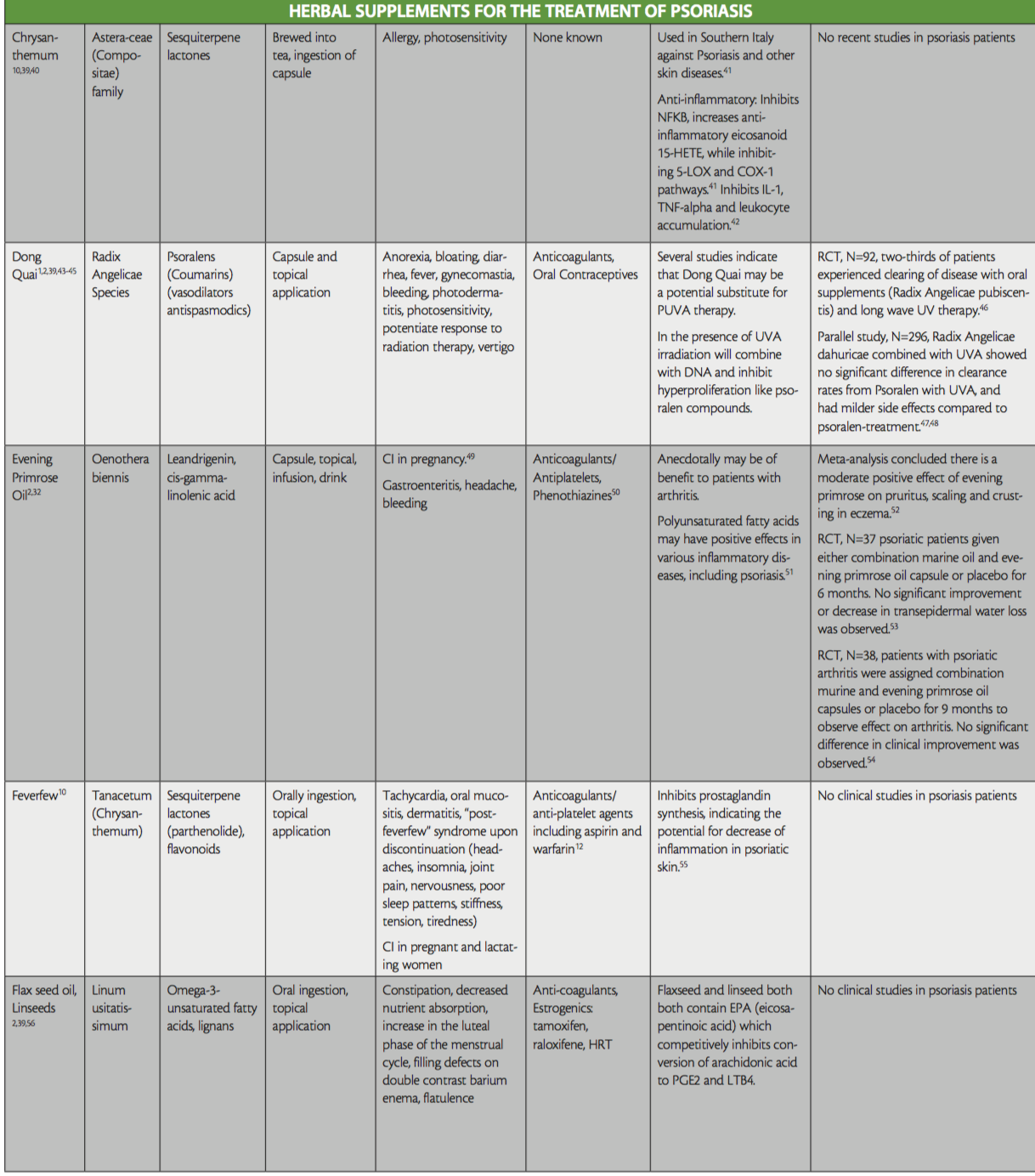
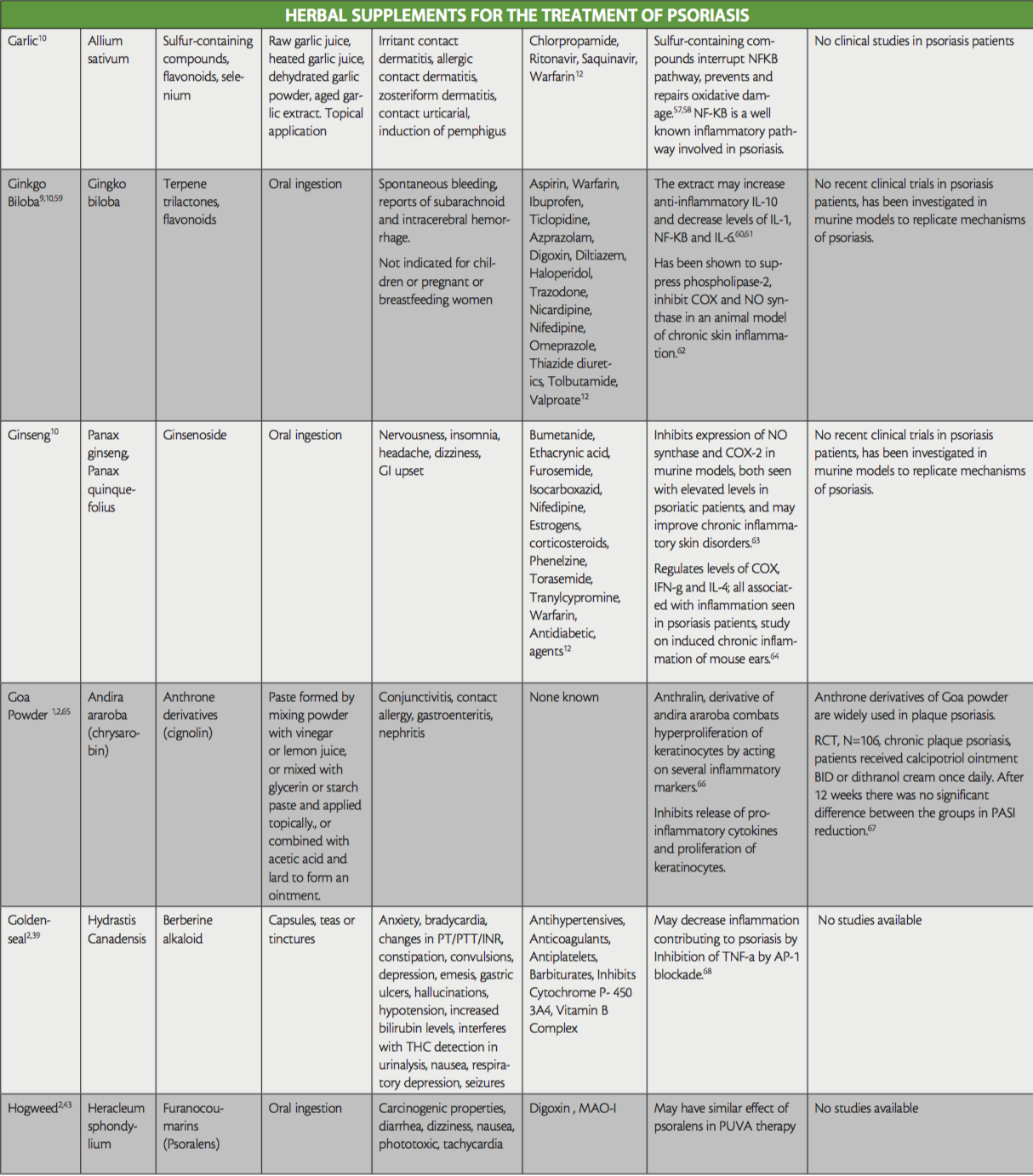
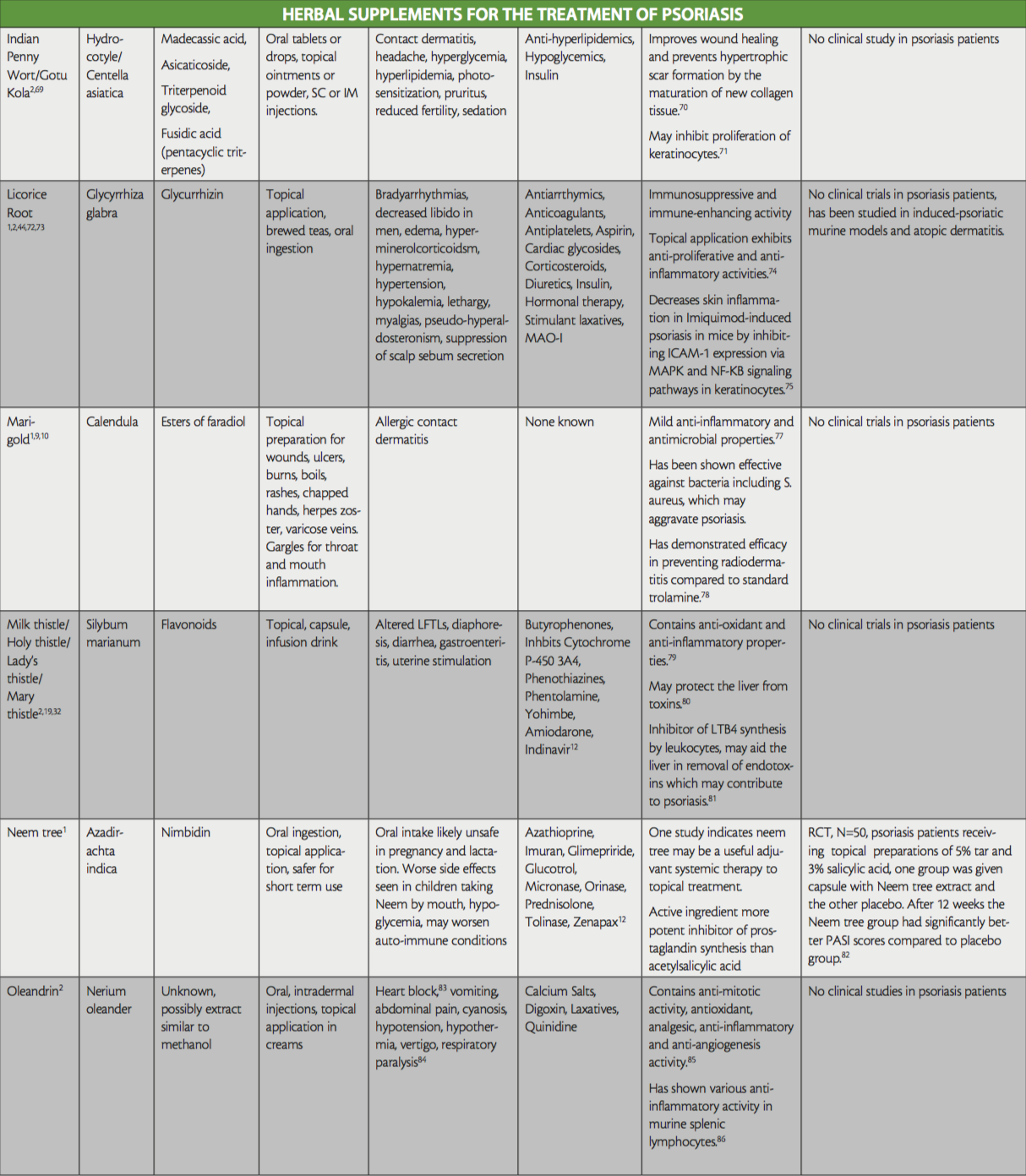
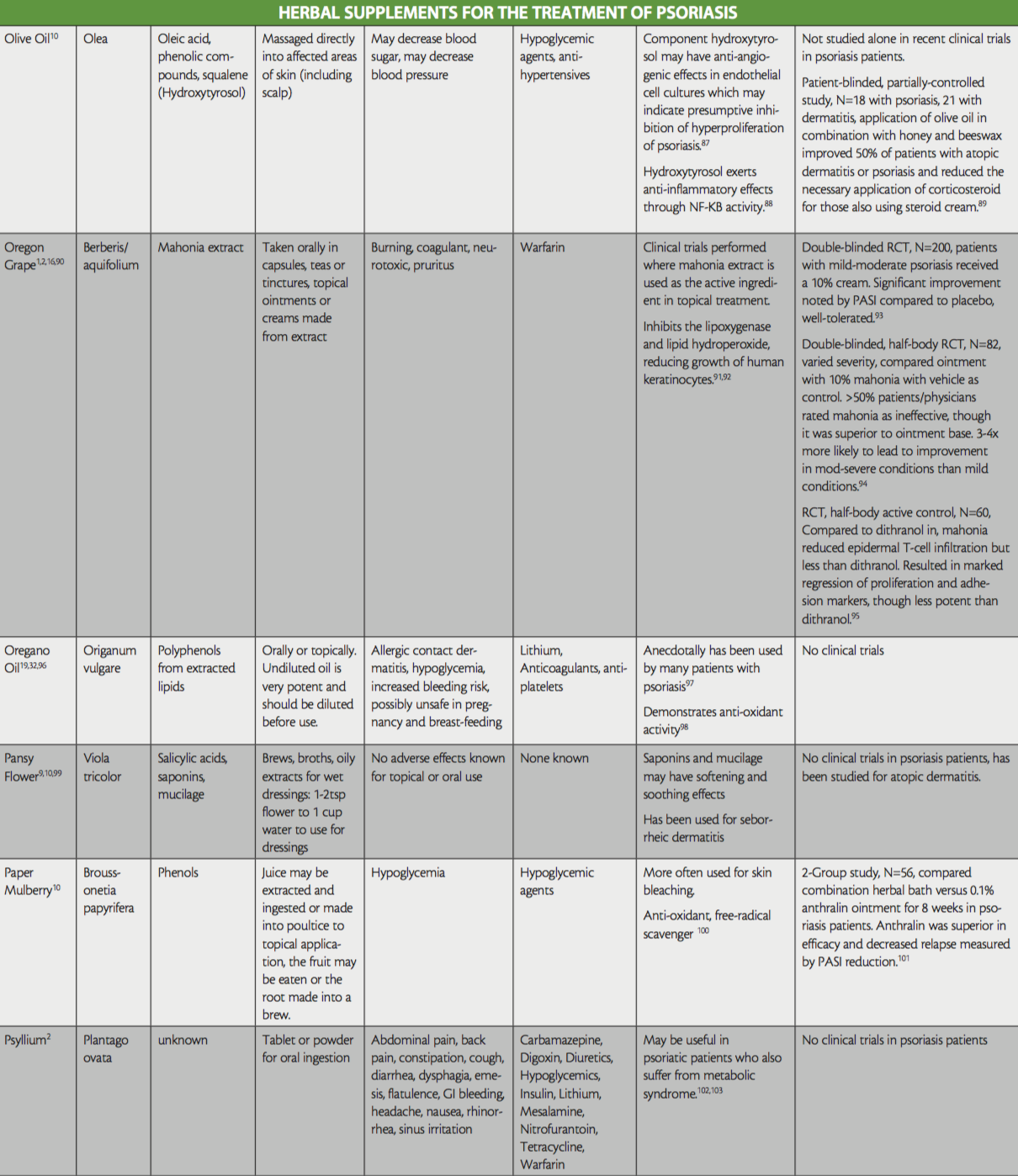
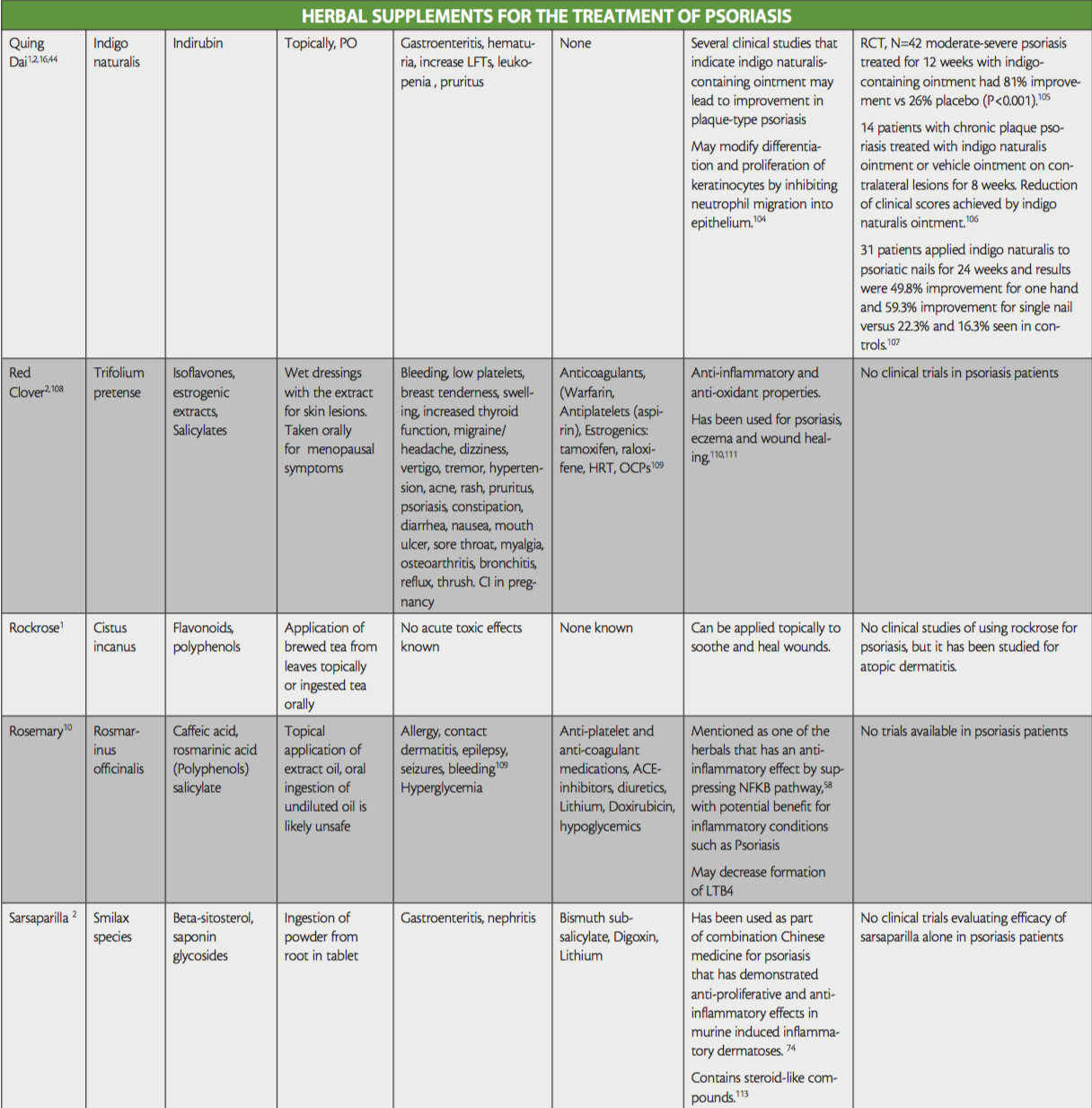
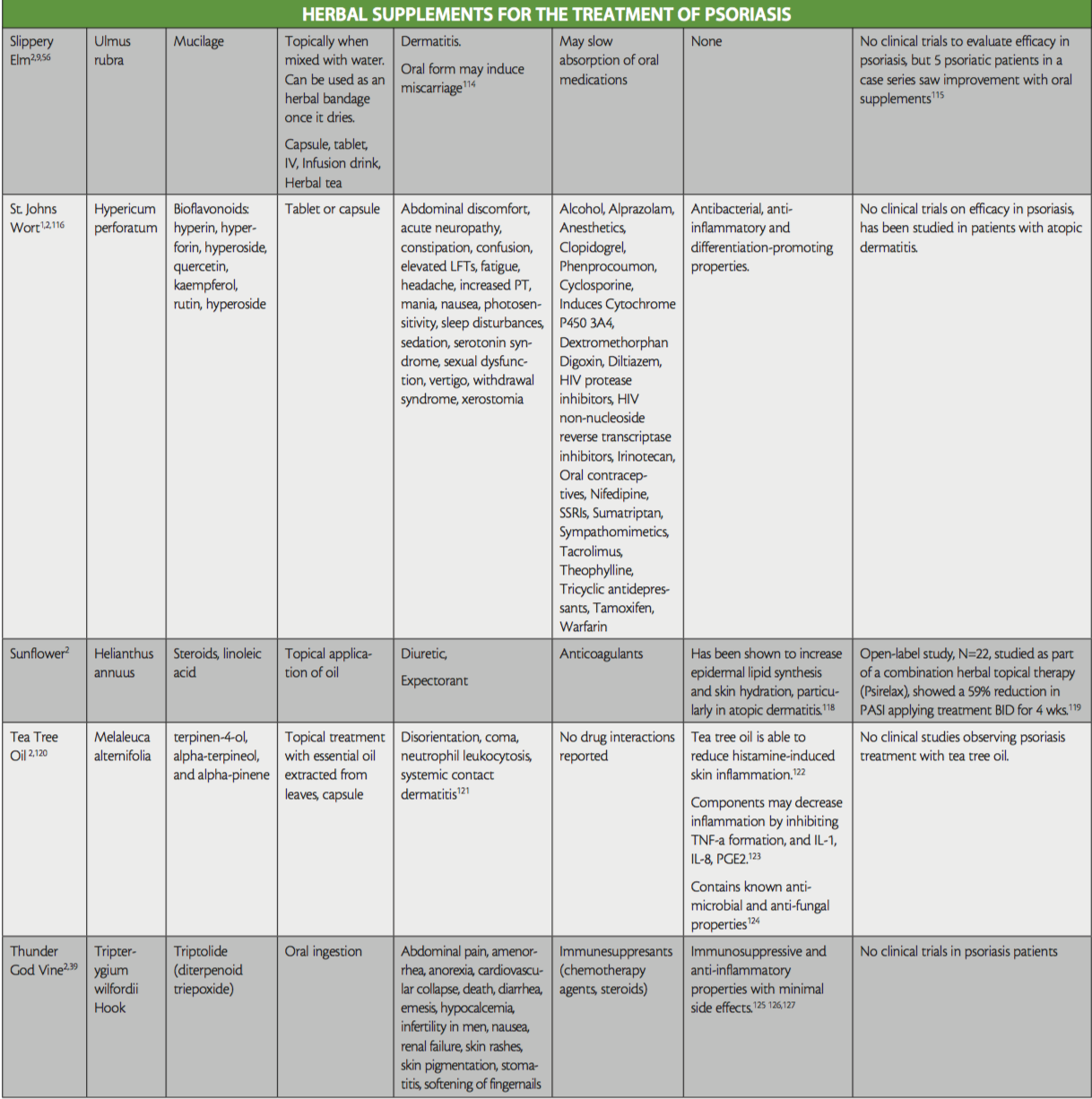
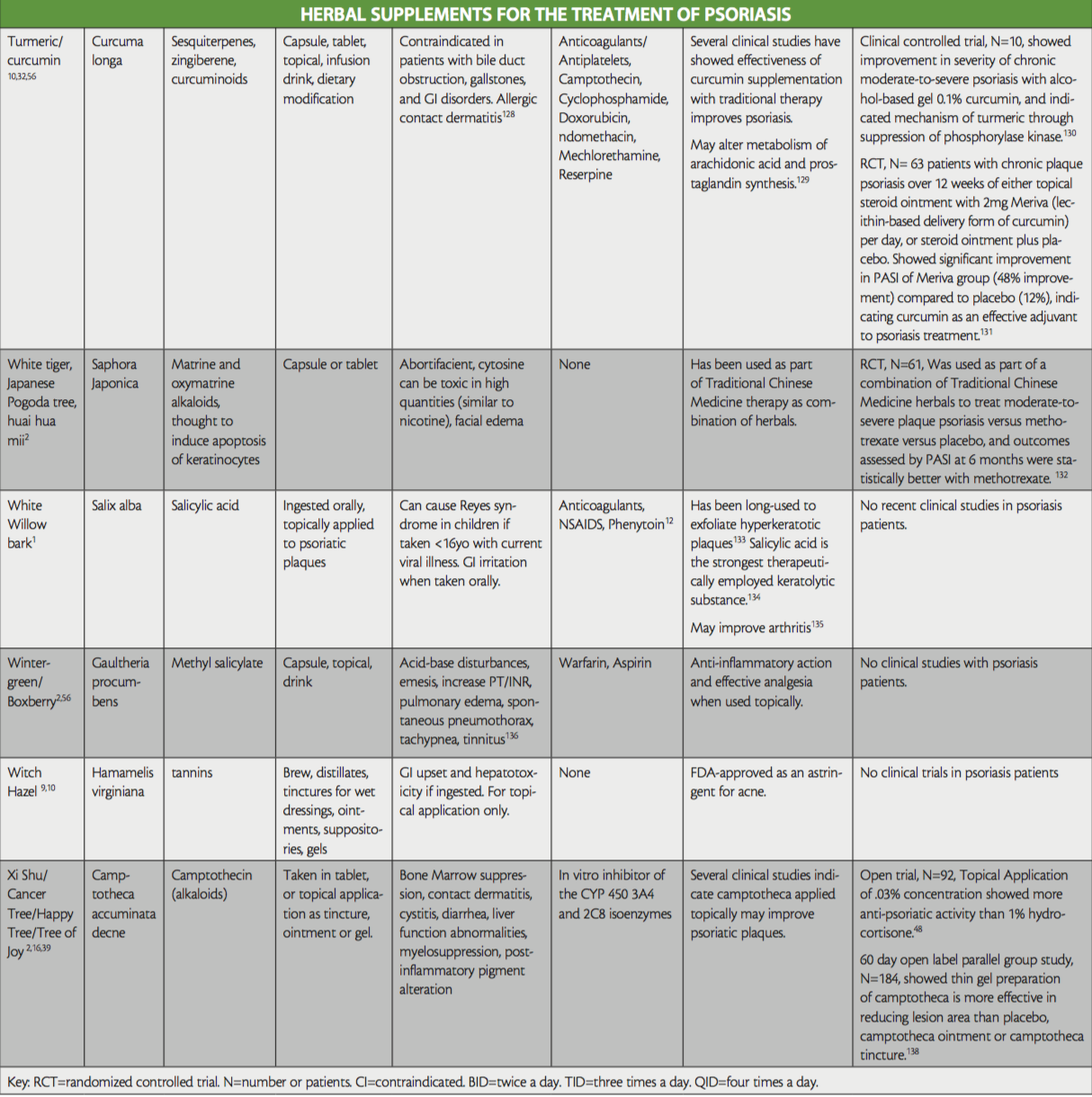
While not all-inclusive, the purpose of this ‘at-a-glance’ reference table is to raise awareness of the herbal treatments that are used in psoriasis, to aid providers treating patients that are currently using or interested in the addition of herbals to their therapy regimen, as well as shed light on any existing evidence for their use. Provided also are their active ingredients, side effects, and potential interactions with conventional medication. Readers are directed to key resources such as websites by WebMD and Medscape, which both offer information on herbal supplements, their side effects and medication interactions.
Financial disclosure/conflict of interest: Hannah Hill and Mona Malakouti have no conflicts of interest and no disclosures. Dr. Anderson serves as investigator on Psolar study Janssen and speaker (Stelara), speaker also AbbVie (Humira), Amgen (Enbrel), Celgene (Otezla), Leo (taclonex and picato). Dr. Jacob was the Coordinating Principal Investigator on the PREA-1 and PREA-2 Trials supported by Smartpractice USA and serves as a consultant to Johnson and Johnson, Inc.
Hannah Hill, BS, Loma Linda University, School of Medicine, MS4, Loma Linda, CA
Nancy Anderson MD, Loma Linda University, Professor, Director of Psoriasis Clinic, Loma Linda, CA
Mona Malakouti MD, Internal Medicine Preliminary Internship, Huntington Memorial Hospital, Pasadena, California
Sharon E. Jacob, MD, Loma Linda University, Professor, Director of Contact Dermatitis Clinic, Loma Linda, CA.
1. Cowen, V. S., & Cyr, V. (2015). Complementary and alternative medicine in US medical schools. Advances in Medical Education and Practice, 6, 113–117. http://doi.org/10.2147/AMEP.S69761
2. Harris P, Cooper K, Relton C, Thomas K. Prevalence of complementary and alternative medicine (CAM) use by the general population: a systematic review and update. Int J Clin Pract. 2012;66:915-916.
3. Eisenberg DM, Davis RB, Ettner SL, Appel 5, Wilkey 5, Van Rompay M, et ci. Trends in alternative medicine use in the United States, 1990-1997. JAMA. 1998 Nov 11;280(18):1569-75.
4. Nahin R, Barnes P, Stussman B, B B. Cost of Complementary and Alternative Medicine (CAM) and frequency of visits to CAM practitioners: United States, 2007. Hyattsville, MD2009.
5. The National Health Expenditure Accounts category of “physician and clinical services” includes “Offices of Physicians (including Doctors of Medicine [M.D.] and Doctors of Osteopathy [D.O.])” (North American Industry Classification System, or NAICS, 6211) and outpa- tient care centers (NAICS 6214), (a portion of NAICS 6215).
6. Ben-Arye E, Ziv M, Frenkel M, Lavi I, Rosenman D. Complementary medicine and psoriasis: linking the patient’s outlook with evidence-based medicine. Dermatology. 2003;207(3):302-307.
7. Stein K. Herbal supplements and prescription drugs. A risky combination? J Am Diet Assoc 2000; 100:4 12.; Helwig D. US pharmacy chain tracks customer’s use of herbals. CIVIAJ 2000;162:852.
8. Rachakonda T, et al. Psoriasis prevalence among adults in the United States. J Am Acad Dermatol. 2014;70(3):512-516.
9. Talbott W, Duffy N. Complementary and Alternative Medicine for Psoriasis: What the dermatologist needs to know. Am J Clin Dermatol. 2015;16(147-165).
Recommended
Atopic Dermatitis and Psoriasis: Treatments, Considerations, and What’s Coming
Atopic Dermatitis and Psoriasis: Treatments, Considerations, and What’s Coming
Atopic DermatitisAtopic Dermatitis and Psoriasis: Treatments, Considerations, and What’s Coming
DermWire TV: Maui Derm Highlights, Plus New and Emerging Treatments for HS and Acne
DermWire TV: Maui Derm Highlights, Plus New and Emerging Treatments for HS and Acne
PsoriasisDermWire TV: Maui Derm Highlights, Plus New and Emerging Treatments for HS and Acne
What's New in Topical Treatment for Plaque Psoriasis?
What's New in Topical Treatment for Plaque Psoriasis?
Maui Derm Hawaii 2024What's New in Topical Treatment for Plaque Psoriasis?
PsA-5T-Ds: A New Psoriatic Arthritis Assessment Tool
PsA-5T-Ds: A New Psoriatic Arthritis Assessment Tool
PsoriasisPsA-5T-Ds: A New Psoriatic Arthritis Assessment Tool









