What If It’s Not Atopic Dermatitis?
Atopic Dermatitis (AD) is among the most common dermatologic diagnoses, especially in children. In the majority of cases, AD is a clinical diagnosis characterized by chronic or relapsing and remitting pruritic eczematous lesions.1 History, morphology, and distribution of skin lesions, as well as associated signs and symptoms, most often lead to an accurate diagnosis.2 However, the presentation can be highly variable based on age, ethnicity, or severity, making identification difficult in some cases.3 Given the variability of presentation and commonality of the diagnosis, it is important to recognize features that may warrant further work-up.
The typical patient is a child presenting with cardinal signs and symptoms, including erythematous and pruritic patches in acute lesions, which often progress to dry or lichenified skin secondary to chronic scratching.3,4 These lesions can be seen on any body site, although there is a predilection for flexural surfaces and some age-associated patterns.4 Additionally, AD is often associated with other atopic conditions, such as asthma, food allergies, and allergic rhinitis.2,5
Although AD is a common dermatologic condition, it is important to consider more rare but serious underlying diagnoses. The presence of atypical features including refractory disease, earlier or later age of onset, greater severity, or recurrent infections may suggest a secondary issue or constitute a syndromic phenotype leading to an entirely separate diagnosis.6 As these features may be subtle in nature, this review will outline more rare mimickers of AD, such as immunodeficiencies, malignancies, nutritional deficiencies, and systemic disease, and serve as a guide to recognize when further workup is necessary.
Immunodeficiencies and Immune Dysregulation Syndromes
While the initial presentation of immunodeficiency syndromes can be highly variable, one common feature is the presence of a dermatologic manifestation.7 These manifestations can present on a spectrum of severity, from mild eczematous rashes to life threatening skin infections or desquamation.6,7 Given that the presence of AD may represent an underlying immunodeficiency, physicians must be aware of features warranting further evaluation. These features include the onset of AD within the first few weeks of life, skin abscesses, and alopecia as well as associated features, which may include recurrent infections, poor weight gain, and a variety of extra-cutaneous characteristics uncommon to AD.6,7 As demonstrated in Figure 1, one such immunodeficiency syndrome, Netherton’s Syndrome, may appear as chronic eczematous eruptions.8 Common lab abnormalities for immunodeficiencies include elevated IgE, inflammatory markers, and cytopenias.6,7 The presence of atypical features or associated lab abnormalities may warrant further workup such as testing for specific mutations.

Figure 1. 9-year old with confirmed SPINK5 mutation for Netherton’s Syndrome
Malignancies and Neoplasia
Dermatologic manifestations may be associated with underlying malignancies.9-11 While these manifestations can be sudden and severe eruptions, more subtle cutaneous findings may also be cause for concern.9 For example, cutaneous T-cell lymphoma (CTCL), a malignant proliferation of helper T-cells, most often presents as a conspicuous, scaly, hypopigmented or erythematous rash and is commonly mistaken for AD.9,10 However, unlike AD, the rash is often unresponsive to traditional therapy and classically progresses from patches to plaques. Additionally, as demonstrated in Figure 2, the rash often presents asymmetrically in a “bathing suit” distribution. Common affected sites include the upper legs, buttock, groin, breasts, axilla, and occasionally, the scalp.9,10 Understanding the atypical distribution and patterns of progression may help distinguish CTCL from benign skin conditions such as AD.10

Figure 2. 73-year-old with a history of itchy, eczematous dermatitis with biopsy-confirmed CTCL
Langerhans cell histiocytosis (LCH), characterized by an abnormal proliferation of langerhans cells, is another neoplastic condition that can be misdiagnosed as AD. It most commonly occurs in pediatric populations and its presentation ranges from isolated skin or bone lesions to life-threatening, multisystem involvement.12 Isolated cutaneous disease is common in young children12 and often presents as an erythematous, papular rash on the groin, abdomen, back, or chest.12,13 Additional features include scaly erythematous plaques involving the scalp, eroded inguinal plaques similar to those of a severe diaper rash, petechial or hemorrhagic lesions, as well as mucosal ulcers or gingivitis.12,13 Any combination of these cutaneous manifestations should raise suspicion for LCH.
Carcinoid syndrome is yet another condition that can demonstrate skin changes similar to those seen in AD, including erythema and xerosis.14 Associated symptoms that should raise concern for carcinoid syndrome include cutaneous flushing, bronchospasm, and diarrhea.14 Although multiple myeloma is not classically associated with eczematous skin findings, there have been several case reports identifying adult-onset dermatoses resembling AD preceding the diagnosis.15
Nutritional deficiencies
Vitamin and mineral deficiencies are often recognized by their associated cutaneous findings.15 For example, scurvy (vitamin C deficiency) famously presents with a hallmark of follicular hyperkeratosis and perifollicular hemorrhages.16 However, cutaneous signs of an underlying nutritional deficiency may take the form of a more subtle rash and can be incorrectly diagnosed as AD.16 Particularly, deficiencies of zinc, vitamin A, B6, B2, and B3, may initially present with eczematous lesions.16 Associated features such as glossitis, arthralgias, diarrhea, anemia, or neurologic deficits should raise concern.16 For example, in zinc deficiency, there may be perioral dermatitis in addition to eczematous eruptions accentuated in the intertriginous areas as demonstrated in Figure 3. In young children, this may mimic facial eczema or diaper dermatitis. However, along with these classical distributions, providers should be especially vigilant of patients with risk factors including infancy, pregnancy, alcohol use disorder, vegetarian diet, dialysis, low socioeconomic status, certain medications, and malabsorption or gastrointestinal surgery.16
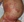
Figure 3. 6-year-old with multiple medical problems and new-onset eczematous eruption with accentuation in intertriginous areas and around mouth. Biopsy supported acrodermatitis enteropathica-like eruption. Zinc levels found to be very low due to improper total parenteral nutrition formulation.
Infections
Infections, such as tinea corporis or scabies, are another potential cause of an AD-mimicking rash. According to one striking study from Brazil, 18% to 43% of children diagnosed with atopic dermatitis actually had scabies.17 While scabies and AD may present similarly, immediate differentiation between the two conditions is imperative for initial management.17 History details, such as pruritus that is worse at night or after a bath, or involvement of the axilla, wrists, or interdigital spaces, as demonstrated in Figure 4, may assist providers in considering scabies.17 In addition, scabies should be considered in cases of intense pruritus that is refractory to AD therapy. Failure to recognize this infestation may cause undue harm to the patient and close contacts, which can result in secondary bacterial infections, insomnia, and stigmatization.17 Furthermore, atopic-like findings are estimated to occur in up to 50% of pediatric patients ultimately diagnosed with HIV.18 While uncommon in the pediatric population, any concerning history or associated symptoms, such as recurrent infections, should warrant further workup.

Figure 4. A 4-year-old with an itchy eczematous eruption refractory to treatment. Scraping revealed scabies infestation.
Systemic Disease
Other chronic or systemic diseases, including thyroid dysfunction, diabetes mellitus, iron deficiency anemia, chronic kidney disease, and celiac disease, can present with cutaneous manifestations similar to AD.19-23 Patients with significant risk factors, atypical skin features, or extra-cutaneous symptoms should be further investigated. Obtaining a full review of systems may uncover a series of features suggestive of an entirely separate diagnosis. Table 1 summarizes the skin manifestations and clinical features of several of these conditions.

Workup
When evaluating patients with a concern for an underlying condition mimicking atopic dermatitis, it is important to consider conditions such as immunodeficiencies, malignancy, nutritional deficiency, and other systemic disease. One should always obtain a detailed history and a thorough review of systems to identify other symptoms. Additionally, while performing the skin examination, checking for the presence of dermatographism can assist in categorization. Especially in refractory cases, the workup outlined in Table 2 may be a starting place.

Conclusion
Atopic dermatitis is commonly seen in clinical practice. Diagnosis is typically based on history and physical exam and, given its prevalence and most often benign course, further diagnostic efforts are generally not required. However, when coupled with atypical features, refractory disease, or extra-cutaneous symptoms, AD may be a manifestation of another underlying condition. The workup depends on the presentation and symptoms but may involve blood work, imaging, skin biopsy, or infectious disease testing. Many of these underlying conditions have treatment methods that often improve cutaneous symptoms. While vigorous diagnostic enthusiasm is often unnecessary for this common skin condition, AD may present a unique opportunity for the perceptive clinician to find more.
1. Eichenfield LF, Tom WL, Chamlin SL, Feldman SR, Hanifin JM, Simpson EL, et al. Guidelines of care for the management of atopic dermatitis: section 1. Diagnosis and assessment of atopic dermatitis. J Am Acad Dermatol. 2014;70: 338–351.
2. Frazier W, Bhardwaj N. Atopic Dermatitis: Diagnosis and Treatment. Am Fam Physician. 2020;101: 590–598.
3. Rudikoff D, Lebwohl M. Atopic dermatitis. Lancet. 1998;351: 1715–1721.
4. Pugliarello S, Cozzi A, Gisondi P, Girolomoni G. Phenotypes of atopic dermatitis. J Dtsch Dermatol Ges. 2011;9: 12–20.
5. Irvine AD, McLean WHI, Leung DYM. Filaggrin mutations associated with skin and allergic diseases. N Engl J Med. 2011;365: 1315–1327.
6. Gaudinski MR, Milner JD. Atopic Dermatitis and Allergic Urticaria: Cutaneous Manifestations of Immunodeficiency. Immunol Allergy Clin North Am. 2017;37: 1–10.
7. Minegishi Y, Saito M, Tsuchiya S, Tsuge I, Takada H, Hara T, et al. Dominant-negative mutations in the DNA-binding domain of STAT3 cause hyper-IgE syndrome. Nature. 2007;448: 1058–1062.
8. Guerra L, Fortugno P, Pedicelli C, Mazzanti C, Proto V, Zambruno G, et al. Ichthyosis linearis circumflexa as the only clinical manifestation of Netherton Syndrome. Acta Derm Venereol. 2015; 95(6): 720-4.
9. Elmer KB, George RM. Cutaneous T-Cell Lymphoma Presenting as Benign Dermatoses. 15 May 1999 [cited 9 Jan 2022]. Available: https://www.aafp.org/afp/1999/0515/p2809.html#afp19990515p2809-b4
10. Mahajan VK, Chauhan PS, Mehta KS, Sharma AL. Poikiloderma vasculare atrophicans: a distinct clinical entity? Indian J Dermatol. 2015;60: 216.
11. Pimpinelli N, Olsen EA, Santucci M, Vonderheid E, Haeffner AC, Stevens S, et al. Defining early mycosis fungoides. J Am Acad Dermatol. 2005;53: 1053–1063.
12. UpToDate. [cited 12 Jan 2022]. Available:
13. Simko SJ, Garmezy B, Abhyankar H, Lupo PJ, Chakraborty R, Lim KPH, et al. Differentiating skin-limited and multisystem Langerhans cell histiocytosis. J Pediatr. 2014;165: 990–996.
14. Kleyn CE, Bell H, Postin G, and Wilson N. Cutaneous manifestations of the malignant carcinoid syndrome. JAAD. 2004; 50(3): P113.
15. Behera B, Pattnaik M, Sahu B, Mohanty P, Jena S, and Mohapatra L. Cutaneous manifestations of multiple myeloma. Indian J Dermatol. 2016; 61(6): 668-71
16. Galimberti F, Mesinkovska NA. Skin findings associated with nutritional deficiencies. Cleve Clin J Med. 2016;83: 731–739.
17. Banerji A, Canadian Paediatric Society, First Nations, Inuit and Métis Health Committee. Scabies. Paediatr Child Health. 2015;20: 395–402.
18. Rudikoff D. The relationship between HIV infection and atopic dermatitis. Current Allergy and Asthma Reports. 2002; 2: 275-81.
19. Verduzco HA, Shirazian S. CKD-Associated Pruritus: New Insights Into Diagnosis, Pathogenesis, and Management. Kidney International Reports. 2020;5: 1387–1402.
20. Ress K, Annus T, Putnik U, Luts K, Uibo R, Uibo O. Celiac disease in children with atopic dermatitis. Pediatr Dermatol. 2014;31: 483–488.
21. Ai J, Leonhardt JM, Heymann WR. Autoimmune thyroid diseases: etiology, pathogenesis, and dermatologic manifestations. J Am AcadDermatol. 2003;48: 641–59; quiz 660–2.
22. Diabetic skin disease. [cited 13 Jan 2022]. Available: https://dermnetnz.org/topics/skin-problems-associated-with-diabetes-mellitus
23. Skin manifestations of haematological diseases. [cited 13 Jan 2022]. Available: https://dermnetnz.org/topics/skin-manifestations-of-haematological-diseases
Ready to Claim Your Credits?
You have attempts to pass this post-test. Take your time and review carefully before submitting.
Good luck!
Recommended
- Infections & Infectious Disease
A Nose for Disease: A Review of Olfactory-Based Diagnosis in Dermatology





